|
However, there was a significant positive correlation between the pupillary responses to phenylephrine and tyramine, ruling out any functionally caused "denervation" hypersensitivity in the dilatator muscle of the iris. Nor was there any positive correlation between the ciliospinal reflex response and the pupillary response to phenylephrine, contradicting an increased density of postsynaptic monoaminergic receptors in the dilatator muscle of the iris as the explanation. According to these premises, a positive correlation should be expected between the ciliospinal reflex response and the pupillary response to tyramine, if the enhanced ciliospinal reflex response was due to an increased presynaptic release of monoamines. The instillation of a 1% phenylephrine solution into the conjunctival sac induces mydriasis by stimulating postsynaptic adrenergic receptors in the dilatator muscle of the iris, while the instillation of a 2% tyramine solution causes mydriasis by releasing noradrenaline from the presynaptic sympathetic nerve terminals in the iris. Tentatively, it may be due to an increased release of monoamines from post-ganglionic sympathetic nerve endings or an increased density of postsynaptic adrenergic receptors in the dilatator muscle of the iris. 
Therefore, the presence of this reflex dose not always preclude a state of brain death.Īn amplified ciliospinal reflex response has been documented in patients with cluster headache, lacking a Horner-like syndrome. Because of the latter pathway to the spinal center, this reflex might remain in patients in whom the brain stem is completely nonfunctioning. A noxious stimulation to the face will be registered through the brain stem, but if stimulation is in the neck or upper trunk, it may go directly to the spinal center. 
The center of the ciliospinal reflex lies in the first three segments of the thoracic spinal segments and two pathways are involved in this reflex. Although brain death was suspected in both cases from its clinical courses, the fact that the ciliospinal reflex was present in each case kept us from declaring that these patients were in the state of brain death. They were the cases of a 74-year-old woman who suffered a right putaminal hemorrhage and that of a 28 year-old male with severe head and cervical cord injury. 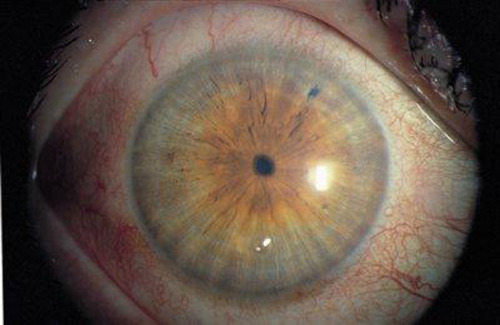
We reported two cases in which the ciliospinal responses judged to be present resulted in the authors' indecision in determining brain death. In the Japanese guideline for determining brain death, the absence of this reflex is considered essential. This reflex is used as an indicator of brain stem and autonomic nervous system functioning. The ciliospinal reflex was first described by Budge in 1852.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
